Blog
This month, we dedicated time to reflect on what it means to live in our current “VUCA” times: a period marked by volatility, uncertainty, complexity, and ambiguity.
This month, we dedicated time to reflect on what it means to live in our current “VUCA” times: a period marked by volatility, uncertainty, complexity, and ambiguity.
Halloween season is full of parties, events, and activities for families, but they are not always accessible or inclusive for neurodivergent and disabled children and their families. That’s why the Center for Connection is bringing back its Inclusive Trunk or Treat event for the 4th year in a row!
This month, we had the honor of welcoming two guest presenters: Noelle Wittliff, LMFT, and Caroline Carter, PsyD, co-authors of a forthcoming book that introduces a new framework for understanding gender development through the lens of whole-brain integration.
On the first Monday of each month, our interdisciplinary team is led by none other than our founder, Dr. Tina Payne Bryson—New York Times best-selling author of The Whole-Brain Child and No-Drama Discipline—in a powerful training experience that brings the latest brain and attachment science and strategies into our work, along with a whole lot of heart.
To our community, our hearts and thoughts are with you during this time. Many of us have been impacted by the recent fires and we hope that you and your loved ones are staying safe. Below is a list of resources our team has pulled together, and we’ll work on adding additional links and supports as soon as we can.
As a business based in Pasadena, The Center for Connection has been significantly affected by the Eaton Fire. A number of our team members and their immediate families have actually lost their homes. We’ve been asked how people can offer assistance, so here are some places you can give support if you’d like.
To our community, our hearts and thoughts are with you during this time. Many of us have been impacted by the recent fires and we hope that you and your loved ones are staying safe. Below are some tips and scripting to help you navigate this situation as a caregiver.
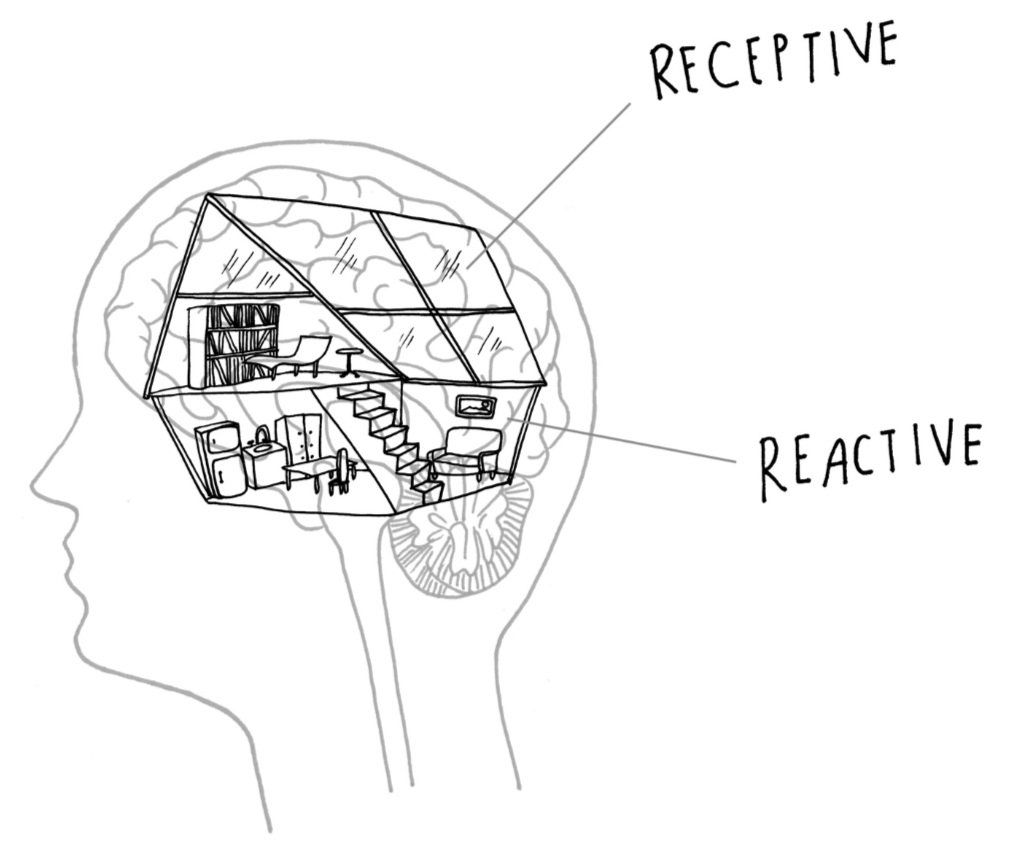
At the Center for Connection, our interdisciplinary approach allows us to paint with a broad brush when working with clients and supporting them in their goals. For example, in a case where the client presents with ADHD and depression, a frequent recommendation might be to recommend Dialectical Behavior Therapy (DBT). However, at the CFC, we might view this client's needs differently and consider more “bottom up” and “top down” strategies.
Resources
Resources for Coping with Coronavirus
Summary Guide for The Power of Showing Up
Summary Guide for The Yes Brain
Summary Guide for No-Drama Discipline
Summary Guide for The Whole-Brain Child
A note to caregivers (ideal for letting caregivers know about your discipline approach)

















![[Repost from The Washington Post]: For queer families, back-to-school time is especially fraught](https://images.squarespace-cdn.com/content/v1/553927d0e4b0b0c45454d21f/1584651956654-Q40HLLODNGHJFDVHG9AL/Screen+Shot+2020-03-19+at+2.05.47+PM.png)










Now is a great time to reach out. We offer psychotherapy, assessments, educational therapy, play therapy, parent support, occupational therapy, and speech and language therapy for clients of all ages.